I had cancer. But you probably already knew that.
But if you didn’t, here’s the only place where I’m going to tell this entire story. Some parts of it may squick you out. I’m warning you up front. Read beyond this point at your own risk!
While I will probably reference my cancer in casual ways throughout the blog (especially as it relates to how I have eaten, my time management, and the fact that I had to take 8 weeks off of work), this is the only place I will go through the entire story. I’m human. I’m still processing what happened to me. Some days I will want to talk about it. Some days I will want to talk about anything but. On those days, you’ll get linked back to this page. I tried to be as honest and forthcoming as I could in the telling of this story. Forgive any inaccuracies in scientific information. I am simply relaying information as I understood it.
You should be warned that this story gets descriptive (I refuse to use the word “graphic”) in parts. Reader discretion is adviced.
The Intraductal Papilloma
Are you one of those people who believes all things happen for a reason? I do. For the purposes of this story, let’s assume all things happen for a reason (just imagine it if you don’t believe).
That being the case, the intraductal papilloma is the place where this story starts.
Warning: Squicky moment #1 ahead.
What the hell is an intraductal papilloma? That’s probably what you are asking. And with good reason. I had no idea what one was until I experienced it.
Without getting into too many cringe-worthy details, an intraductal papilloma is a little cauliflower-like growth that can develop inside a milk duct. It doesn’t hurt. In and of itself it isn’t (necessarily) a signal of cancer. If you have one, though, there’s one distinct thing you might notice. Your nipple will bleed.
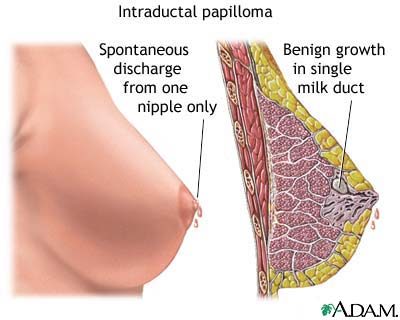
That’s what happened to me. And I’m not talking a tiny dot or anything. I’m talking about “I could wet nurse a baby vampire.” So you could understand how this freaked me out.
Both my grandmother and my great-aunt (maternal) both died from breast cancer so I take breast stuff way seriously. At the time I had no idea what an intraductal papilloma was but I did know that one is not supposed to bleed from the nipple, especially fourteen years after the last time they’ve given birth to anybody!
So I went to see my gynecologist and reported the problem. They ordered a mammogram, which came back confirming the papilloma. But for some reason they sent me back for another mammogram (which baffled me, the radiology company, and my insurance) just to make sure. Still I complied. Same result. I was referred to a breast surgeon who then wanted me to do another mammogram. One thing you should know about me? I have no tolerance for medical shenanigans. They make me shut down. So that’s exactly what happened, especially after the surgeon told me that papillomas are basically harmless. I didn’t feel like getting another mammogram so I just didn’t.
And fourteen months passed.
How Nik’s Procrastination Actually Paid Off For Once
Fast forward to November 2015. It had been a few years since I’d had a primary care physician. (I know, I know…) So I asked a few friends for recommendations. I was very specific about the kind of doctor I wanted. Pardon my French, but I told my friends, the doctor needed to be, “No non-sense, able to see through my bullshit and who will nag me relentlessly to do what I’m supposed to do.”
My good friend Dee recommended her doctor to me. He was everything I could have hoped for. The man came into the room with his questions and his stethoscope and whatnot. We went through every little problem I’ve ever had. And he ended the session with an action-item list.
It’s like the man knew me in another life.
One of those action items was that I had to revisit the papilloma. He agreed that it was probably harmless (and I remember that word “probably” because it stuck out to me) but that for my own comfort I should get it resolved. I agreed. So he referred me to another breast surgeon in the same medical system and off I went.
When I went to go see that breast surgeon, he had a very practical reason for me to need to do another mammogram – it had been fourteen months since my last one.
Now let’s pause here and talk about mammograms because there are two main types and they are not the same. I’m going to give you my understanding of the distinction between the two (if I got something wrong or missed something, please leave it in the comments!).
- A routine mammogram is done on both breasts and takes images of your breast tissue, which a radiologist examines for any general abnormalities. If he finds none, you are off the hook for a year.
- A diagnostic mammogram may be done on either both or just one of the breasts, and when they are done, the radiologist may look at specific parts of the breast for an already identified problem. This may or may not be paired with an ultrasound reading.
So I went to the mammogram and met a radiology technician who I now call my guardian angel. She was about my mom’s age, had that wry sense of humor and had been through enough mammograms herself to know what a pain in the butt they are. I will also digress for a moment to say that for me while mammograms were a pain in the butt, they were never painful. Uncomfortable? Yes. Painful? No.
Moving on. So they did the diagnostic mammogram and they saw the papilloma but they saw something else. Tiny calcium deposits throughout my breast. I did not know this at the time but those can be a pre-cursor to breast cancer. So an ultrasound was ordered. And as the radiologist looked at my breast her grimace got deeper and deeper. She told me I needed to get back to see my breast surgeon as soon as I could and not to delay. There were several red flags that needed to be investigated.
I say that my procrastination paid off for once because the papilloma drove me to the breast surgeon. The breast surgeon discovered my cancer. To be sure, some of those precursors were there in my mammograms from fourteen months ago, but my surgeon is fairly sure I had not developed cancer at that point. So that papilloma? Probably saved my life.
Two biopsies, an aspiration and a lumpectomy
So I returned to see my breast surgeon who explained to me they saw a lump that needed to be investigated. Besides that I appeared to have the early signs of breast cancer. So it was really, really, really important that I follow through with these tests. (By the way, I hadn’t told them about my propensity to flake out of medical stuff, but damn was I appreciative of how hard they leaned on me to do what I was supposed to do!)
There were three things that needed to be done:
- Something called a stereotactic biopsy, to examine the calcium deposits in my breast. Because they are so tiny, it takes special machinery to do this biopsy.
- A regular biopsy to remove a portion of the lump they found.
- A lymph node aspiration to see if there was abnormal cell activity in my lymph nodes.
My surgeon said he was fairly sure I had what is called Ductal Carcinoma in Situ (DCIS). This is considered Stage 0 breast cancer and is highly treatable (as long as you don’t flake on your treatment!)
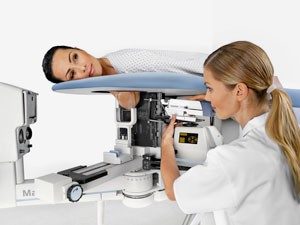
The biopsies were an adventure. Let’s talk about the stereotactic first. It basically involves laying on a table that is raised up off the ground. You lie face down. There is a hole in the table through which you put the breast in question. Below the table there is what I can only assume is a really big needle. (They numbed me) and an imaging machine. The imaging machine finds the calcium deposits, the needle goes in to extract tissue containing the calcium deposits. I did my lump biopsy that same day as well.
And inextricably both biopsies came back normal. I had the lymph node aspiration. That came back normal.
My surgeon was quick to temper any hopes that this meant I was cancer free. “This just means we have not found it yet. You have cancer. It is in there somewhere,” he said.
Can I just explain to you for a moment how it feels to hear that? You have a deadly disease inside of you, but we can’t quite find it. And if that disease grows it could potentially kill you, did we mention that? It was nerve-wracking to say the least. I was comforted by the fact that it was such an early stage that they had trouble finding it but on the same token, I really needed them to find it! So we scheduled a lumpectomy to remove that whole lump to be tested. And that is when they found the cancer.
BRCA1 and BRCA2
Believe it or not, I was relieved by my diagnosis. Mostly because the thought of having cancer in me and not knowing where it was was akin to walking through a mine field. At least after my diagnosis we knew what and where it was.
Immediately after my diagnosis I was scheduled for what was called a Multi-Disciplinary meeting (or Multi-D for short). This is where my breast surgeon and several oncologists lay out every test result and they look at my family history (which was mostly oral history that I gave) and they determine their recommendation for my treatment. Ohhhhh, I was ready for them.
This section could have easily been called, “Why You Do Not Rely on Dr. Google.” Because Dr. Google did not prepare me for the options I was given! Basically I was given two treatment options:
- They could do an exploratory surgery to make sure they got all the cancer out. (Sidenote: In cancer treatment there is a term called “clearing the margins.” If during your lumpectomy your surgeon clears the margins that means it is apparent that they got all the cancer. If they did not clear the margins that means the caner may have spread. My surgeon did not clear the margins). This would be followed by a course of radiation therapy, possibly hormone suppression therapy, observation every six months for…life. And there was a 35-40% chance of the cancer reoccurring. Or there was the other option which was.
- To have the tissue in both my breasts removed via a bilateral mastectomy.
(Jigga-WHAT???)
That option very much hit me from the left. Dr. Google told me about option #1. The traitor said nothing about option #2! I was stunned. I was speechless (which is rare). The doctors explained that the recommendation came from the fact that I had what was called a “hormone responsive” cancer, which meant that it “fed” on estrogen. So long as I had breasts I’d have an environment where estrogen could aid a cancer in growing again. This is why they suggested in option #1 that I’d have to do hormon suppression therapy. I’m still about 10-ish years from menopause so I still have plenty of hormones to worry about.
Seeing that I was overwhelmed, and in an attempt to cajole me out of my shell-shocked state, my breast surgeon mentioned that I also had the right to get genetic testing for the BRCA1 and BRCA2 genetic mutations.
You may know what this is because of Angelina Jolie. She tested positive for the genetic mutations (she got tested because her mother died of breast cancer). The mutations mean that you have a higher-than-normal chance of developing breast and ovarian cancer (don’t quote me but I believe it’s an 80% chance). If you have the BRCA1 or 2 genetic mutation, that starts a chain of events to protect you and your family from those cancers. I say your family because if you have other family members, it is recommended they too get tested if you have a positive result, especially female family members (like my two daughters an my niece). My doctor also told me that if I had the genetic mutation my gynecologist might recommend that I have my ovaries removed.
So that all is totally not overwhelming, right?
But I went for the testing and there were some reassuring things I learned. For example 95% of breast cancer cases are not associated with BRCA 1 or 2. So the genetic mutation is actually quite rare. With my familial history, though, the genetic counselor I saw agreed it was prudent to test me. So she took a swab from my cheek and we hoped for the best. What I didn’t tell anyone was that that was going to be my litmus test for if I should do the mastectomy. (At least at that point it was.) If I didn’t have the mutation, I’d do treatment option #1. If I did have it, I’d do treatmetn option #2.
But I started to rethink that as time went by. I mean the result was important, but at that point it was more important to my family than it was to me. I’d already gotten breast cancer, so what did knowing that I was 80% likely to get it really mean in the grand scheme of things? It would help determine if I needed to have my ovaries removed but besides that I came to the conclusion that it probably wasn’t the best way to make my decision.
And besides, both tests came back negative. (Hooray!)
Free Boobs
You may wonder how I ended up making the decision to have the mastectomy.
I can’t really explain how I made that decision. I did all the requisite things: pro’s/con’s list, I prayed about it, talked with friends, talked with people who had undergone breast cancer treatment. In the end I asked myself what felt right. When I thought about the radiation therapy and living my life around the notion that cancer could come back, that made me antsy. The thought of the mastectomy made my a bit nervous too but I realized it was mostly because I didn’t know much about the process. So I began asking questions.
I learned that after a breast cancer diagnosis, my insurance had to cover reconstruction of both breasts even if the removal of the second breast was prophylactic (to prevent the development of a future cancer). So I was referred to a few plastic surgeons. I met with them all and settled on a super nice, but very quiet surgeon. I liked him because he took a lot of time to talk me through my situation and all my choices. It seemed like at every step on the road of this thing I was presented with many choices and it got overwhelming.
Sidebar: Can I just say that it takes a good amount of emotional fortitude to go for a plastic surgery consult? It’s true. Consider the set-up:
- You go into an exam room and you have to stand partially unclothed (in my case, topless/braless) for a long period of time
- Then the surgeon does what I call “the 360,” examining you from all sides. My surgeon was quiet as he did this, occasionally extracting a tape measure to make some obscure note, other times, simply lifting flaps of skin and saying, “hmph.”
- Then he takes pictures of you from all angles.
- Finally, you go back to his office where guess what is waiting for you. Guess. I’m gonna tell you. A big ass screen with all the pictures of you in your flabby fabulousness!
This crap isn’t for the faint of heart.
So anyway…because I’d experienced massive weight loss in the regions that I did (stomach, back, etc.) I had a few options for reconstruction.
- Just implants. I could have the tissue removed from my breasts and simply get implants. Pro’s: This was the most technically simple option and the shortest surgery. Con’s: Not really a con but there’s always a risk that there won’t be enough viable skin to cover an implant or that the skin they leave can become necrotic (die) which would mean the implants would have to come out and I’d have to wait six months before attempting further reconstructive options.
- TRAM Flap. Basically this involved the surgeon taking my pannus flap (excess skin in my stomach area, or my “apron”) and pulling it up to my breast area to form new breasts out of them. Pro’s: Very natural look which doesn’t necessarily need an implant. Also sort of like getting a bonus tummy tuck for free. Con’s: They stretch out your abdominal wall which weakens it and that is irreversible. My surgeon said things like doing crunches and heavy weight lifting might not be possible.
- Latissimus Dorsi Flap: This is where they take excess skin from the back area and bring it around to the front to construct a breast. Pro’s: again very natural and not as much worry about muscle weakening as the TRAM flap. Con’s: It’s a long surgery and long surgeries carry increased risk of infection and death.
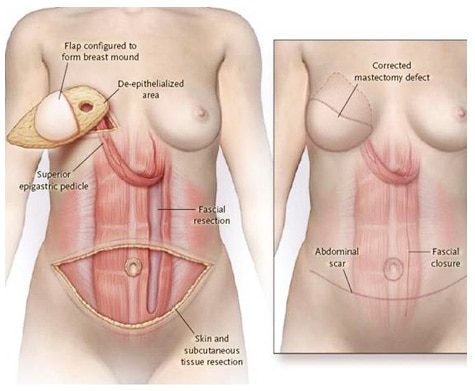
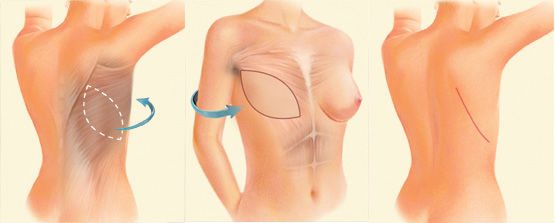
And there you have it! My next set of stressful choices. But these were slightly easier for me. I knew the TRAM was out. I didn’t like the idea of that irreparable weakening in my abdominal wall. Your core muscles are too important to too many things! That left implants or the Latissimus Dorsi (NOTE: The Latissimus Dorsi could also be paired with implants). In the end, I gave authorization for the implants but if there wasn’t enough skin to do just the implants, I wanted the Latissumus Dorsi flap. There, decision made.
One note. Warning: Another squicky moment ahead. Because they had to take all the cancerous tissue out that meant they would not be able to leave my nipples. That was a weird thought for me. Nipples are…well…they are your nipples! You are supposed to have them, right? This tidbit about the nipples will come in handy in a moment.
Telling Everyone
Up until this point there was only a very close circle of friends who knew what was going on. That was good. I couldn’t handle people’s advice and certainly not their sympathy or empathy at that point. I have to shout out my good friend Dee (the one who referred me to my now PCP). She went to every appointment with me an remembered to ask all the questions I was too shell shocked to ask.
But after I made the decision to have the mastectomy, I realized I had to tell other people. Like my children. And my family.
Surprisingly most everyone was pretty chill about the news. They were worried and thankful it was caught early. They were unsure about the surgery. The only person who had a complete freak-out was my dad. And who could blame him. When you hear the word “cancer” come out of your only child’s mouth that has to be panic-inducing. But still. I’m glad I gave myself ample time to absorb the news myself before having to relay it.
That’s an interesting thing about this process. I found myself consoling others a lot about my diagnosis. I told them “there, there…” “it’ll be ok…” But here’s the deal: I was the one with cancer! More than one person said I seemed “stoic.” I’m going to choose to take that as a compliment. I was freaking out. But I gave myself the privacy to freak out before dealing with the rest of the world.
I also decided I’d be pretty open about it in the #FoodieNation. To be clear I probably didn’t have to be. Nowadays there is a #TeamFoodie. Shannon runs the Facebook page and Julia picks up the slack with a private Facebook group I run (it’s currently full but keep a lookout because I will notify folks when spots become available). So far as blog posts, I have enough recipes on this site to keep everyone occupied a very long time.
But still. I wanted to be open for few reasons:
- I consider the #FoodieNation my family. And family shares stuff with family.
- I knew by this time this was more emotionally than I knew what to do with. I’d need help processing.
- I knew this was more logistically than I could handle. I’d need help! (Not necessarily from the#FoodieNation but from my Facebook friends at large)
So one day I decided to hit record on my phone and I did it. I made the whole announcement. It was cathartic to get it out into the world. And what I got back was so, so, so good. Love. From everyone. From everywhere. Lots of love. Overwhelming love. Hugs and love and prayers and light. It was just so much. And I needed it. So I was glad I decided to tell everyone.
“I Still Have a Nipple…”
So the day of the surgery arrived. May 5. My brother and his family came into town. I tried to argue him down that it wasn’t necessary but he wasn’t having it. My brother is nine years younger than me but he’s an old soul. He’s already lost a sibling (on his father’s side) and he’d be damned if he’d let me go into surgery without hugging me and telling me he loved me.
My dad also came into town. It was interesting to have all that family gathered around me for this event. Up until the moment I walked into the operating room (and we’re getting to that but I did, in fact, walk there) it was all hypothetical.
The morning of my surgery was somewhat stressful. What I haven’t told you throughout was that there was a “side story” going on in my life. My boyfriend (who lives with me) has advanced kidney disease as a result of diabetes. So he had to start dialysis. Which meant just days before my surgery, he went for outpatient surgery to get set up for dialysis (he’s also on the transplant list). So…there was that. He was supposed to accompany me to the hospital for my surgery. My best friend was to drive us. But the night before he’d felt really unwell and took pain meds to help and…well…I couldn’t get him awake!
So I just left. My best friend could not sit with me because he had to work that day. Which meant I arrived to the hospital alone. To have a bilateral mastectomy.
And I even managed to hold it together for about 25 minutes through getting registered. I furiously dialed my friend Dee to see if she could come down and sit with me until surgery but it was super early in the morning. In desperation, I called my brother (who I love but is not necessarily the person I wanted with me as surgeons marked up my breasts to prep me). Everyone was still asleep.
I arrived at the surgical center and was greeted by a nurse who took my vitals and then by my very chipper plastic surgeon who bid me good morning aaaaaaand…
I lost it.
I started crying. And not just crying. Hysterically crying. A hysterical, gutteral, body-quaking, hyperventilating, face swelling, nose-running, “trying to speak is futile because it all becomes one, long, unintelligible word” crying.
He was a bit concerned.
For me, this was the moment when all that stress came out. Up until then I’d relied on research and support to make decisions, but that was in fact my only goal. Make the decisions. I wasn’t being very mindful of my heart and soul, which is very important in these situations. I think what I’ve learned over the past few years is that I relied on my late mother a lot for that sort of stuff. She’d be the person who would needle me. “How are you, Nikki? No really. Not what you tell other people. This is me. How are you???” And because she was my mother I would tell her. When I was said I sad I was sad. When I was scared I’d say I was scared. When I wanted my mommy, I would say I want my mommy.
And that morning, so very desperately, I really, really, really wanted my mommy. And yes, she’s always here with me in spirit but that’s not what I mean. I wanted her there. Arms wrapped around me, smelling of Boucheron perfume and baby powder, using her perfectly manicured nails to stroke my hair and say, “it’s ok baby. It’s going to be just fine. Mama’s here.”
But I didn’t have that. So I cried. Hysterically.
My surgeon didn’t miss a beat either. He immediately hugged me (which was a bit awkward because at this point I was shirtless for him to mark me). Then my general breast surgeon came in and he consoled me too. By that time my sister-in-law called me back that she was on her way to the hospital. It was a relief when she got there. She didn’t do anything special. She was just there. Sometimes you just need somebody to be there.
The hospital where I had surgery is big into informed consent so along the way I was asked a bunch of times what procedure I was having, who I was, yadda. Finally, it came time to go to the operating room. Here’s how that went down. They wheel you to the O.R. but they stop just outside it. You get off the gurney and walk into the room. There are nurses and my surgeon and the anesthesiologist all waiting for me. I said to them, “My name is Nikki Massie and I’m here today to have a bilateral mastectomy with reconstruction.” And that’s precisely what happened.
Man. Anesthesia. It’s trippy. Even being a writer I cannot accurately convey what the experience of going under general anesthesia is like, but if you’re reading this you’ve mostly likely done it. The thing that weirds me out the most is that you just cease to exist for a number of hours. It’s like you blink and it’s five hours later and your body is profoundly different. That’s what happened to me. I noticed two distinct things almost immediately after I awakened from surgery:
- A sharp – and I mean sharp – pain in my rib cage when I tried to breath in.
- I still had one of my nipples.
Both those sensations were a bit overwhelming and so I tried to hold my breath to get a handle on the pain. My O.R. nurse quickly kiboshed that though and gave me pain meds. After a while they wheeled me in my room where my boyfriend and Dee and my brother and his wife were all waiting for me. And in my hazy state I called Dee over, because really she was the only person to whom I could say this (and even in my hazy state I knew that). She came over and leaned toward me and I whispered into her ear.
“Dee. I still have a nipple.”
The Rest
I think I’m going to draw this very long post to a close. But I will say recovery from any surgery is hard and this one was no exception. I had four drains from the surgery, one of which I had to keep for a month until it smelled like something from The Walking Dead (ew). My incisions tried to be difficult in closing and it took me a while to get a handle on my pain. It also took a while for any sensation to come back in my chest area, which was very, very weird. I couldn’t even feel my own skin.
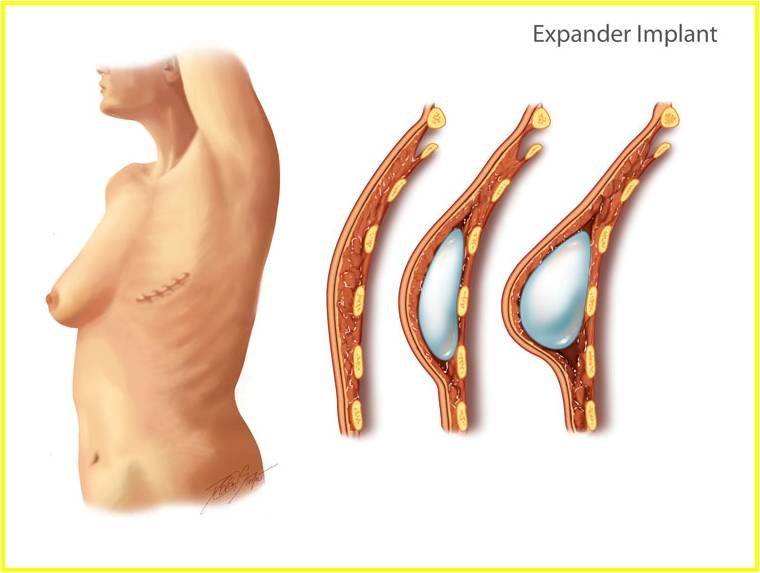
The way the surgery turned out, they were able to reconstruct my left side. I now have an implant (and all the requisite perkiness that comes along with it). On the right side I have what is called a tissue expander, which is a balloon type apparatus that sits under the skin and into which you insert fluid to stretch out the skin so that there is enough to cover an implant. It was weird to me that they had to do that. Prior to surgery I was a size 48 H cup bra. After surgery I was a 38 DDD. But the amount of skin they had to take to protect me from cancer was substantial. I also had more surgery on that side because they took what is called my sentinel lymph node. Basically they lymph nodes hang out in clusters (I think of them like grapes). The sentinel protects the others. So if there is no cancer in the sentinel, there’s no cancer in the others.
Thankfully there was no cancer in the sentinel node but there was still a bit in my breast. But the oncologists felt comfortable that my surgeon got it all and I do not have to undergo any further cancer treatment. I look forward to having my right breast reconstructed at the end of this year (by then my skin will finish stretching and I will have built up enough leave time to take off to recover).
This has been a journey for me. And what I have told you was just one dimension of my life. During that time I also worked full time up until my surgery, bought a house, experienced a major catastrophe with the house that had to be repaired before my surgery and another two catastrophes after my surgery. Plus managing my daughter going to her prom and my boyfriend starting dialysis.
I have said it before and I’ll say it again. I am not extraordinary. I am a regular person with regular capabilities. I had my fair share of meltdowns throughout this whole thing. But you know what? I came through the other side. I hope that serves as a comfort to you if you are going through stress or hard times. If I – imperfect and scattered as I am – can come through all this and still be around to write this freakishly long blog post? There’s hope for all of us.
Addendum: The Right Boob Debacle
So…as I write this section, it is three years to the week of my initial diagnosis. I think I’m finally ready to talk about what happened after my mastectomy. And there is much to talk about.
Let’s start with the hospital bill.
I can’t even explain how this happened except that I was stressed and not on top of my game (and not really great at medical due diligence in the first place) but my plastic surgeon was not covered by my insurance.
So six weeks after my mastectomy, I got a bill for $25,000. Yeah.
I was shocked and scared and traumatized (on top of the trauma I’d already experienced…you know…having cancer). And everyone pointed the finger at everyone else. My surgeon’s office pointed the finger at the insurance company, asking why they sent an approval letter if they weren’t going to pay the bill. My insurance company (rightfully) pointed out that the surgeon’s office should know which insurance plans they are approved to accept. In the middle was me, who does not have $25,000 laying around.
What saved me, in the end, were the disclosure forms.
I signed many disclosure forms leading up to my surgery and one of them was a financial disclosure that listed my financial liability at $2,500 (the amount of my annual deductible) with the rest being billed to insurance. Begrudgingly, the surgeon’s office had to honor that and wrote off the rest of the cost of my surgery. But that wasn’t an instant process. I actually went through my employee assistance plan to get a nurse advocate. I highly recommend them! I signed a paper giving her permission to act on my behalf and, like a little bulldog, she went to every doctor, nurse, and secretary and got this all sorted out. I am eternally thankful for her!
So I paid my deductible and the office said they’d also honor my second reconstructive surgery (on the right boob) with the same agreement. It all seemed too good to be true.
It was.
After about six months with the tissue expander, I went back to my surgeon to start the process of getting an implant on my right side. We went through all my options and in our final meeting he asked if I had any questions. I said yes.
“I’d just like to re-confirm the details of our payment arrangement one more time so that I understand it.” He grimaced. “Come again?” he said.
I explained to him the conversation that had gone down between his office staff and my nurse advocate. I had an email confirming it all and I showed it to him. The color drained from his face. He excused himself.
He came back in with his billing person who kept throwing me eye daggers as she explained that “I know how the situation is handled, right?” I responded by showing her her own email. The color in her face drained. They both excused themselves.
In the next room I could hear the surgeon talking very sternly to his staff. While I couldn’t make it all out, a few things seemed apparent:
- He was never told about the first billing issue.
- He was not consulted about the payment arrangement we ultimately did for the first surgery.
- He seemed most upset that they had gotten my hopes up for something that couldn’t happen (also he seemed upset by legal liability).
So after a few moments he comes back in and, in his kind way, tells me he cannot perform the second surgery. He cannot absorb the cost. His staff would help me find a surgeon on my insurance he’d personally talk to that surgeon (as many plastic surgeons are not apt to take over a case). More stress on top of stress.
His office proved to be unhelpful in my search for a new surgeon (I think they were maybe mad I got them in trouble). I found a good surgeon on my plan and, as it turns out, this surgeon interned with my surgeon decades ago, so they knew each other. I facilitated the conversation between the two of them and we arranged for me to do a consult.
Save the nipple
There were philosophical differences between surgeon #1 and surgeon #2. For example, surgeon #2 was perplexed about why surgeon #1 saved my nipple. From my surgical notes, he said my nipple would have been highly at risk for necrosis (dying), so he basically said surgeon #1 was just that good of a surgeon to have kept it alive. I thought to myself, “Well…there’s that…”
Except there was more. There always is.
Since my surgery my left side settled and you could see the surgeon left too much skin there (I’ll spare you any pictures). So there is this round orb of a breast with a big puddle of skin hanging off of it. My poor nipple is hanging on for dear life and when I’m upright it’s almost underneath my breast. Surgeon #2 proposed fixing that (which my insurance would cover) but with one caveat: he did not feel he could save the nipple again and he wasn’t apt to try.
So…there I was…with another decision to make.
And it may seem trivial to you. It’s a nipple. No big deal, right? But here’s the thing: to this day it remains the ONLY thing in my chest area I can feel. The only thing that makes my breasts seem like a real part of my body. Had surgeon #1 taken the nipple, I would have dealt. But knowing what it feels like to have absolutely no sensation across an entire swath of your body except one spot? Yeah. You get protective of that spot.
So, to his chagrin, I chose to leave my left breast alone and simply swap the expander on the right for an implant. To be clear, this bugged the crap out of him. He’s a plastic surgeon. His aim is perfection and I would not be perfect. Surgeon #2 was generally a nice guy, but I could tell my decision greatly bothered him, as evidenced by the fact that when he recorded notes on my visits he made sure to point out that it was my choice not to further reconstruct my left side. But anyway…
In December of 2017, I checked in to get my right side done. It was outpatient surgery and it was much easier (both the surgery and the recovery) than the mastectomy. I think the biggest problem I had afterward was that I stopped drinking caffeine while recovering (not intentionally, I just did) and got a whopper of a headache! But finally…I had two boobs.
Granted, they do not match. They don’t even have the same brand implant in them. And, honestly, I’m thinking that after the 10 year shelf-life of these implants I may just go flat. I’ve learned in the past three years these boobs are not what define me!
In the end, I’m not sorry for any of the decisions I made, though. I don’t know if I could have handled going flat from day one. I think that it would have done a psychological number on me. So I am glad I tried reconstruction. I have learned a lot from it. There are a few lasting effects. Because of the extent of surgery on my right side and the way they manipulated my muscles for reconstruction, it is ridiculously easy to pull my neck (as in, it happens virtually every day).
But guess what? I’m here. I’m cancer-free. And, if I have anything to do with it, I’m going to spend the remainder of my life being healthy so that I can, in fact, achieve my goal of being a kick-ass great grandma.
Because that’s worth fighting for.
Ok…NOW the story is over! Go schedule your yearly mammogram, ladies. 😉



Nikki, though I followed your journey with cancer throughout, this is very well written, and filled in the few blanks. I think you are an extraordinary human being and I love you! I am so very happy that you have come through this with flying colors! ??. Many hugs to come in August!!
All I’m going to say is God bless you Nik! You have always been such an inspiration to me and are even more so now. I’m keeping you and your family in my prayers and I pray your boyfriend’s wait isn’t long. My husband was on the liver transplant list for a little over 4 months 4 years ago. Thankfully his wait was short and I pray the same for him.
Thank you for telling your story. I cried when you wrote about your Mom. So very touching.